Consider the following:
You seem to be getting enough sleeping, you eat pretty normally, nothing is obviously wrong, yet your battery seems stuck at 60%. Workouts feel heavier. Your brain feels a half-step slower. You are the person reaching for a sweater when everyone else is fine.
Online, people often call this “mitochondrial dysfunction.” It’s a useful phrase, but it can also be misleading, because it can sound like a diagnosis. It isn’t.
What it usually points to is a pattern, a cluster of experiences that can happen when your overall energy system has less capacity or resilience than than what you expect.
Let’s translate the biology into what it actually feels like in real life.
First, what mitochondria do
Mitochondria are the main sites where cells turn fuel and oxygen into ATP, your body’s usable energy currency. ATP helps power muscle contraction, nerve signaling, organ function, and the quiet background work of keeping you alive.
But mitochondria do more than just “make energy.” They also:
- influence how cells respond to stress
- help regulate redox balance and signaling
- coordinate quality control, recycling damaged parts and building new capacity over time (PMC)
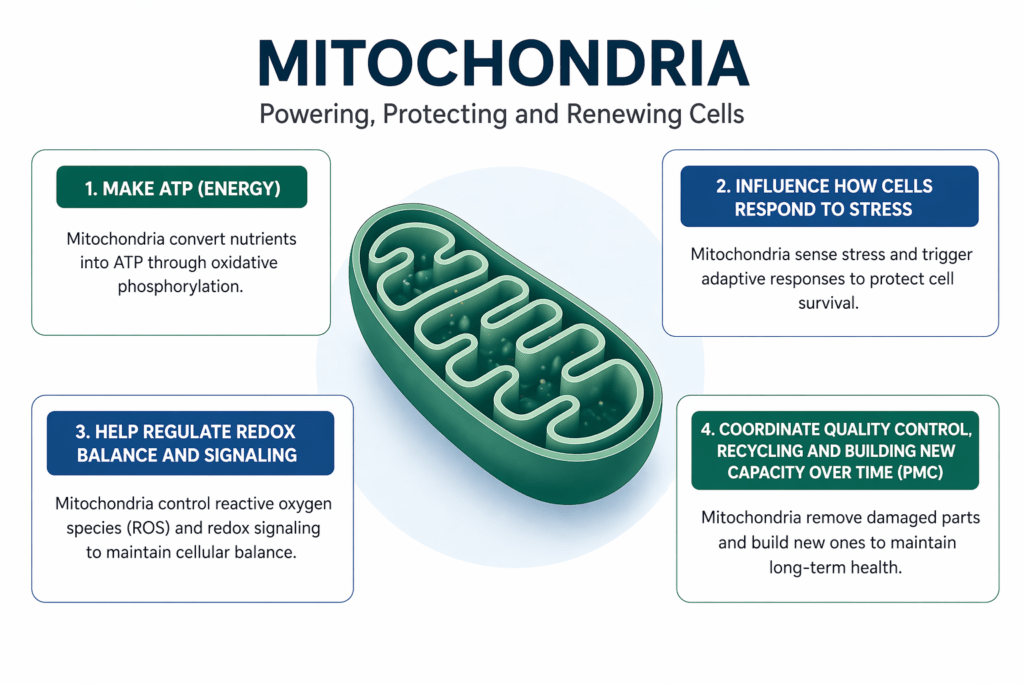
What this means in real life is simple: mitochondria are part of why you can meet a demand, then recover, then do it again tomorrow.
The “low mitochondrial capacity” pattern
You can’t feel what your mitochondria are doing directly. What you can feel are the downstream effects when energy supply and stress tolerance don’t match the demands of daily life.
A low mitochondrial capacity pattern often shows up as:
- reduced stamina (physical or mental)
- higher perceived effort for normal tasks
- slower recovery after exertion
- more sensitivity to sleep loss, under-fueling, illness, or stress
None of these are proof of mitochondrial dysfunction but they are clues that your system may be running at a lowered capacity.
Fatigue that feels disproportionate
A classic description is not just “tired.” It’s tired relative to what you did.
You might notice:
- you crash after a day that used to feel normal
- you need more breaks to keep the same pace
- caffeine helps the feeling, but not the underlying capacity
Researchers studying fatigue across conditions have repeatedly explored mitochondrial bioenergetics as one contributing factor, especially because fatigue often behaves like a mismatch between demand and cellular energy availability. The evidence is mixed and context-dependent, but it is a serious area of investigation. (PMC)
Why this matters: Disproportionate fatigue is often the first sign that your recovery “budget” is getting tight, regardless of the root cause.
Poor recovery and exercise intolerance
One of the most mitochondria-linked lived experiences is exercise intolerance, a reduced ability to sustain activity at the intensity you expect, sometimes followed by an unusually long recovery.
In primary mitochondrial diseases, fatigue and exercise intolerance are common and well described. (PMC) In everyday life, the same shape of experience can appear for many reasons, but mitochondria are a plausible contributor because skeletal muscle relies heavily on mitochondrial oxidative phosphorylation for sustained work.
What it can feel like:
- your legs “burn” earlier than expected, for example when climbing stairs
- you hit a ceiling quickly even at moderate pace
- you feel wiped out for longer than your peers after similar training
- soreness and heaviness linger, even when the workout was not extreme
At the tissue level, muscle fatigue is not just one thing, it is a combination of fuel use, ion balance, nervous system output, and cellular energy pathways. Mitochondrial capacity affects how much work you can do aerobically and how efficiently you restore balance afterward. (MDPI)
Why this matters: Recovery is where you build capacity. If recovery is chronically underfunded, fitness and resilience can stall even with “good” effort.
Brain fog and low mental stamina
Brain fog is a fuzzy term but when discussing it, people tend to mean:
- slower recall
- reduced focus
- lower tolerance for multitasking
- feeling mentally drained faster than usual
Neurons are energy-demanding cells, and mitochondrial function is tightly connected to synaptic activity, signaling, and cellular stress handling. This is why mitochondrial disruption is a recurring theme in research on aging and neurodegeneration. (PMC)
That does not mean everyday brain fog equals neurodegeneration. Much more often, brain fog reflects sleep debt, stress load, inflammation after illness, medication effects, or under-fueling. Still, it is reasonable to say that if your cellular energy system is strained, your brain is one of the first places you notice it.
Why this matters: Mental stamina is a form of metabolic stamina. If your day demands constant attention, you need more than grit. Your biology needs real recovery.
Cold sensitivity and low heat output
Some people with low energy availability describe feeling cold easily, especially:
- after poor sleep
- during dieting or low-carb phases
- when training volume is high
- when stressed or run down
Body temperature regulation is complex, but mitochondria sit near the center because heat is a metabolic byproduct, and in specific tissues like brown adipose tissue, mitochondria can actively produce heat through uncoupling mechanisms (often discussed in the context of UCP1 and cold adaptation). (PMC)
In humans, brown fat activity and cold adaptation vary widely between individuals and contexts. So cold sensitivity is not a clean “mitochondria test,” but it can be useful as part of the broader pattern when overall energy throughput is low.
Why this matters: If you are consistently cold plus fatigued, it is a signal to zoom out to sleep, fueling, stress, and basic health labs if appropriate.
A key reality check: the same symptoms can come from many causes
It’s important to note that fatigue, poor recovery, brain fog, and cold sensitivity are non-specific.
They can reflect:
- sleep disruption or circadian misalignment
- low iron or anemia
- thyroid dysfunction
- inadequate calorie or protein intake
- overtraining or under-recovering
- depression, anxiety, chronic stress
- infections and post-viral states
- cardiopulmonary limitations and other medical issues
So we should treat “mitochondrial dysfunction” as a lens, not a label. If a symptom cluster is persistent, worsening, or limiting daily life, it is reasonable to talk with a qualified clinician.
What tends to improve mitochondrial capacity over time
If you want the most evidence-aligned way to support mitochondrial function, it is not a hack. It is the unglamorous basics that repeatedly show up in human physiology research:
Build aerobic capacity gradually
Endurance training is a well-established stimulus for mitochondrial biogenesis and improved oxidative capacity in skeletal muscle, especially when progression is sustainable. (PMC)
Practical translation:
- start where recovery is easy
- add volume slowly
- keep some sessions truly low intensity
Respect recovery as a biological process
Mitochondria are involved in muscle repair and regeneration signaling. When you stack stress without recovery, you can feel the gap. (PMC)
Practical translation:
- plan rest days like you plan workouts
- watch the “2-day rule,” if you are still crushed two days later, that dose may be too high right now
Sleep is mitochondrial support, indirectly but powerfully
Sleep affects hormonal regulation, appetite signals, and stress physiology, all of which change energy availability and perceived effort. Sleep is not “mitochondrial” in a simple way, but it strongly shapes the environment mitochondria operate in. (Read more)
Fuel the work you ask your body to do
Under-fueling can look like “low mitochondria” quickly: cold sensitivity, low drive, poor training response, and persistent fatigue. Matching intake to output is not just about performance, it is about having enough substrate to adapt.
Why this matters: Mitochondria respond to the whole environment, training, sleep, nutrients, stress hormones, and inflammation. Capacity is built system-wide.
For a more detailed look at how you can improve mitochondrial function, read our article How to Repair and Maintain Mitochondrial Health Naturally.
結論
Low mitochondrial function does not always feel dramatic. Often, it feels like reduced margin in your energy levels.
You can still get through the day but every exertion seems like it costs more. Workouts feel heavier. Recovery takes longer. Focus fades sooner. Sleep loss, stress, illness, or skipped meals hit harder than they used to.
That does not mean every low-energy pattern is due to mitochondrial dysfunction. Fatigue, brain fog, cold sensitivity, and poor recovery can come from many causes. But mitochondria are part of the energy system that helps your body meet demand, adapt to stress, and recover afterward.
The most useful takeaway is not to self-diagnose. Instead, notice the pattern and rebuild capacity over time through steady movement, adequate fueling, sleep, recovery, and a broader strategy for cellular energy support.
For people thinking seriously about mitochondrial health, Mitozz fits into that broader conversation. Developed by FMG Health Sciences, Mitozz contains 98% pure (−)-epicatechin, a compound studied in relation to cellular signaling pathways involved in metabolism, circulation, and mitochondrial function. It is not a shortcut around the basics, but it may be part of a more complete approach to supporting energy, resilience, and healthy aging.
このブログ記事をシェアする
参考文献
- Alway, S. E., et al. (2023). The Role of Mitochondria in Mediation of Skeletal Muscle Repair. (Review). (PMC)
- Cai, Q., & Tammineni, P. (2017). Mitochondrial Aspects of Synaptic Dysfunction in Alzheimer’s Disease. (PMC)
- Filler, K., et al. (2014). Association of mitochondrial dysfunction and fatigue. (ScienceDirect)
- Mancuso, M., et al. (2012). Fatigue and exercise intolerance in mitochondrial diseases. (PMC)
- Yoneshiro, T., et al. (2025). Brown fat thermogenesis and cold adaptation in humans. (PMC)
- Wang, G., et al. (2019). Regulation of UCP1 and Mitochondrial Metabolism in Brown Adipose Tissue. (MDPI)
- Muscular Dystrophy Association. (n.d.). Signs and Symptoms of Mitochondrial Myopathies. (Muscular Dystrophy Association)
ミトコンドリアの健康を理解するには長い時間がかかります。だからこそ、私たちは「Mitozz を立ち上げました。ここは、細胞エネルギーの科学を探求し、生活習慣がミトコンドリアにどのような影響を与えるかを学び、専門家によるディスカッションや教育コンテンツ、ライブQ&Aを通じて最新情報を入手できる、自由な場です。ご自身のペースでご利用いただけます。
Mitozz に参加しましょう
細胞エネルギーとミトコンドリアの健康に焦点を当てた、会員や専門家によるディスカッション、教育コンテンツ、ライブQ&Aセッションをご利用いただけます。
医療に関する免責事項:本記事で提供される情報は、教育および情報提供のみを目的としており、医学的アドバイスを意図したものではありません。専門的な医学的診断、治療、または指導に代わるものではありません。 食事、運動習慣、断食、またはサプリメントの使用を変更する前には、必ず資格を持つ医療専門家に相談してください。特に、持病がある方、妊娠中または授乳中の方、あるいは薬を服用中の方は注意が必要です。
FDA免責事項:これらの記述は、米国食品医薬品局(FDA)による評価を受けたものではありません。これらは、いかなる疾患の診断、治療、治癒、または予防を目的としたものではありません。