Key Takeaways
- PCOS is a whole-body condition that often intersects with metabolic health.
- Oxidative stress and mitochondrial performance are active areas of interest in women’s metabolic health research.
- Simple lifestyle habits like movement, nutrition, and stress management can help support mitochondrial health.
- High-purity (-)-epicatechin, the signature ingredient in Mitozz, is studied for its ability to support mitochondrial biogenesis and the body’s natural antioxidant defenses.
Prefer a quick overview? This video explains how hormones, metabolism, cellular energy, and mitochondria can intersect in PCOS, including why normal energy production matters for everyday vitality.
Now let’s look more closely at the biology behind those connections.
Polycystic ovary syndrome (PCOS) is often discussed as a reproductive diagnosis but a better way to think of it is as a whole-body condition that can involve ovarian function, hormone signaling, and metabolism. This broader view is reflected in the 2023 International Evidence-based Guideline, which emphasizes accurate diagnosis, attention to cardiometabolic and mental health risks, and lifestyle foundations tailored to the individual. (PubMed)
In this article, we will employ a cellular energy biology lens, to make PCOS easier to understand. That includes mitochondria, oxidative stress, and the way cells respond to metabolic demand. Looking at PCOS through this systems lens will help explain why symptoms can cluster and why support often needs to be multi-layered.
PCOS is a whole-body condition, not just “cysts”
PCOS is commonly diagnosed using a combination of features that can include irregular ovulation or cycles, signs of higher androgen activity, and polycystic ovarian morphology on ultrasound. Importantly, having ovarian cysts is not the same thing as having PCOS, and many people with PCOS do not experience PCOS in the same way. (PubMed)
That variability matters. Two people can share a diagnosis while having different dominant drivers such as:
- insulin resistance,
- neuroendocrine signaling patterns,
- inflammation,
- sleep disruption, or
- genetic susceptibility.
This is why PCOS care is increasingly framed around individualized risks and goals, not just one universal protocol.
Why this matters: When you stop looking for a single cause, it becomes easier to focus on the physiological loops that can be nudged over time.
The main physiological loops behind common PCOS features
1) Insulin signaling and androgen activity
Insulin is not only about blood sugar. It is also a growth and signaling hormone that can influence ovarian function. In many women with PCOS, insulin resistance and higher circulating insulin are common, and higher insulin can amplify ovarian androgen production and reduce SHBG, which can increase free androgens. This helps explain why metabolic and androgen-related symptoms often travel together. (PubMed)
Why this matters: When insulin runs high, it can push on the same networks that shape ovarian hormone output, hunger and satiety cues, and day-to-day energy regulation.
2) Ovulation and brain-ovary communication
Ovulation is coordinated by the hypothalamus, pituitary, and ovaries. The hypothalamus and pituitary release signaling hormones, mainly LH and FSH, that help follicles mature and help with ovulation timing. In many PCOS phenotypes, this signaling pattern can shift in a way that increases ovarian androgen production and interrupts normal follicle development, contributing to irregular or absent ovulation. (PubMed)
Why this matters: PCOS is not only an ovarian issue, it is also an endocrine communication issue.
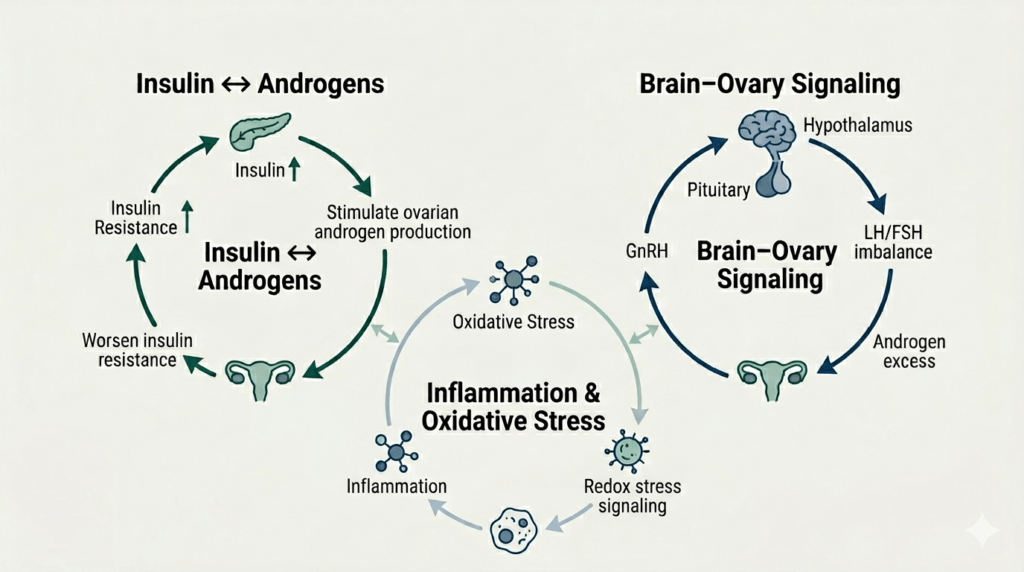
3) Inflammation, oxidative stress, and cellular energy demand
A consistent theme in PCOS research is the presence of oxidative stress signals and low-grade inflammation. Oxidative stress refers to an imbalance where reactive oxygen species outpace antioxidant defenses, which can affect cellular signaling, membranes, and mitochondrial function. (Frontiers)
In ovarian tissue, researchers often focus on granulosa cells, the support cells that help follicles develop. These cells are energy-demanding, and multiple studies and reviews describe mitochondrial abnormalities and oxidative stress markers in granulosa cells from people with PCOS compared with controls. (Frontiers)
This does not prove that oxidative stress causes PCOS but it does suggest that oxidative stress may be part of a reinforcing loop, where metabolic strain increases cellular stress, and cellular stress can worsen signaling.
Why this matters: Cellular energy systems shape how tissues adapt to load. In PCOS, that adaptation may be shifted in ways that are important for both metabolism and ovarian function.
Recap
- Insulin and androgen signaling can amplify each other in many PCOS phenotypes.
- Oxidative stress and mitochondrial signals are commonly observed, especially in granulosa cells, and may be a reinforcing loop.
What is meant by “mitochondrial dysfunction” in PCOS
Mitochondria are often called the “powerhouses” of the cell because they help generate ATP, the body’s energy currency, but they also do something just as important. They serve as a kind of metabolic control room, integrating fuel availability, redox balance, and stress signals.
In PCOS, mitochondrial dysfunction refers to things like
- altered mitochondrial structure,
- changes in mitochondrial dynamics,
- shifts in ATP production capacity, or
- changes in oxidative stress markers.
Reviews summarize these patterns across ovarian tissue and sometimes skeletal muscle and adipose tissue. (Frontiers)
An important thing to consider is a that mitochondria may be both responding to PCOS-related conditions, like insulin resistance and inflammation, AND shaping how cells adapt to that load. When the body is under metabolic stress, mitochondria can send stress signals that influence how cells use energy and respond to hormones.
Why this matters in real life: Mitochondrial dysfunction affects energy availability and cellular stress signaling. In PCOS, that can make metabolic responses less predictable and may contribute to the “whole-body” feel of the condition, going beyond the reproductive symptoms.
Practical foundations for metabolic resilience
The 2023 international guideline highlights lifestyle management as a foundation in PCOS care. (PubMed)
This is because lifestyle inputs like, movement, sleep, nutrition, and stress recovery, are upstream regulators of insulin signaling, inflammation, and metabolic flexibility.
Movement that improves insulin signaling
Exercise is one of the most reliable ways to improve insulin sensitivity and cardiometabolic markers. Meta-analyses in PCOS suggest exercise can improve measures like insulin resistance and body composition, and in some newer syntheses report reductions in total testosterone on average with aerobic training, although results vary. (PMC)
In practice, consistency matters more than perfection. Resistance training and aerobic work can both support glucose handling, mitochondrial adaptations in muscle, and stress resilience, especially when recovery is respected.
Eating patterns that lower metabolic strain
There is no single “PCOS diet” that wins universally. A guideline-aligned approach is to focus on sustainable dietary patterns that support metabolic health and are realistic to maintain. Many people do well with higher-fiber foods, adequate protein, and minimizing ultra-processed foods, but the best approach is individualized. (PubMed)
Sleep and stress recovery as hormone inputs
Sleep and stress are not just side topics, they are hormonal inputs. In the general population, poor sleep can impair glucose regulation and shift appetite signaling, and stress physiology can influence reproductive hormone patterns. PCOS-specific sleep research is still developing, but from a systems perspective, better recovery reduces the background signal from stress and sleep debt, which can make glucose control, stress signaling, and reproductive hormone rhythms easier for the body to regulate.
Where Mitozz fits in
At FMG Health Sciences, we focus on cellular energy because it supports how tissues work and adapt across the body, including in the systems involved in reproductive function. Mitozz contains 98% pure (-)-epicatechin, a plant-derived flavanol studied for how it influences vascular function, cellular stress-response signaling, and metabolism.
Mitozz is designed as complementary nutritional support for people who are interested in supporting mitochondrial health. But there are also other ways to support your mitochondria. If you are interested in learning more, read our article How to Repair and Maintain Mitochondrial Health Naturally.
If you are just starting on your mitochondrial health journey and would like to learn the basics about what mitochondria are, what they do, and how to improve them, check out our Mitochondria 101 page.
Share this blog article
FAQs
Is PCOS the same as having ovarian cysts?
Not necessarily. Polycystic ovarian morphology on ultrasound can be part of PCOS diagnosis, but PCOS is defined by a pattern of features and is not the same thing as “cysts.”
Can Mitozz treat PCOS?
No. Mitozz is a dietary supplement intended to support normal cellular function. It is not intended to diagnose, treat, cure, or prevent PCOS or any disease.
Does exercise really change hormones in PCOS?
Research suggests exercise can improve metabolic markers in PCOS and may reduce total testosterone on average in some studies, but responses vary and results depend on the training program and the individual.
References
- Teede, H. J., et al. (2023). Recommendations from the 2023 International Evidence-based Guideline for the Assessment and Management of Polycystic Ovary Syndrome. PubMed record. (PubMed)
- American Society for Reproductive Medicine. (2023). Recommendations from the 2023 International Evidence-based Guideline for PCOS. (ASRM)
- Gao, Y., et al. (2023). Oxidative stress and mitochondrial dysfunction of granulosa cells in polycystic ovarian syndrome. Frontiers in Medicine. (Frontiers)
- Xie, C., et al. (2023). Mitochondrial abnormality in ovarian granulosa cells… Molecular Medicine Reports. (Spandidos Publications)
- Yan, X., et al. (2025). The role of mitochondrial dysfunction in ovarian granulosa cells… Endocrine Connections. (Bioscientifica)
- Patten, R. K., et al. (2020). Exercise interventions in PCOS: systematic review and meta-analysis. (PMC)
- Atmaca, L., et al. (2025). Effectiveness of exercise interventions on androgen outcomes in PCOS: meta-analysis. Frontiers in Sports and Active Living. (Frontiers)
- McDonald, C. M., et al. (2021). (-)-Epicatechin induces mitochondrial biogenesis… (open-label human study in a specific clinical context). (PMC)
- ClinicalTrials.gov. (NCT01856868). Use of (-)-Epicatechin in Becker muscular dystrophy. (ClinicalTrials.gov)
Understanding mitochondrial health is a long-term process and that’s why we created the Mitozz Community. It’s is a free space to explore the science of cellular energy, learn how lifestyle signals support mitochondria, and stay informed through expert discussions, educational content, and live Q&A—at your own pace.
Join the Mitozz Community
Access member and expert discussions, educational content, and live Q&A sessions focused on cellular energy and mitochondrial health.
Medical Disclaimer: The information provided in this article is for educational and informational purposes only and is not intended as medical advice. It is not a substitute for professional medical diagnosis, treatment, or guidance. Always consult with a qualified healthcare professional before making changes to your diet, exercise routine, fasting practices, or supplement use, especially if you have a medical condition, are pregnant or nursing, or are taking medications.
FDA Disclaimer: These statements have not been evaluated by the Food and Drug Administration. They are not not intended to diagnose, treat, cure, or prevent any disease.






