Key Takeways
- Women’s metabolism changes across life stages.
- Metabolic health is more than weight.
- Mitochondria shape your energy capacity.
- Waist size can matter more than the scale.
- Build flexibility with strength, sleep, food, and recovery.
Women’s Metabolic Health Is a Life-Stage Story
Metabolic health is more than just body weight. It’s about how well your body can sense fuel, store it safely, use it efficiently, and recover after demand. That includes blood sugar control, triglycerides, blood pressure, inflammation tone, and, less visibly, how your cells decide whether to burn fat or store it.
For women, that story has a unique rhythm. Hormones don’t merely regulate reproduction; they also help coordinate energy availability across tissues like muscle, liver, and fat. Pregnancy temporarily rewires metabolism to support a developing fetus. And the menopausal transition shifts the hormonal “settings” that influence where fat is stored, how muscle uses glucose, and how resilient energy systems feel day to day. (Wiley Online Library)
In other words, hormonal transitions and life events can recalibrate fuel use and storage, so metabolic health is dynamic, not static.
The Metabolic Operating System: Mitochondria + Hormones
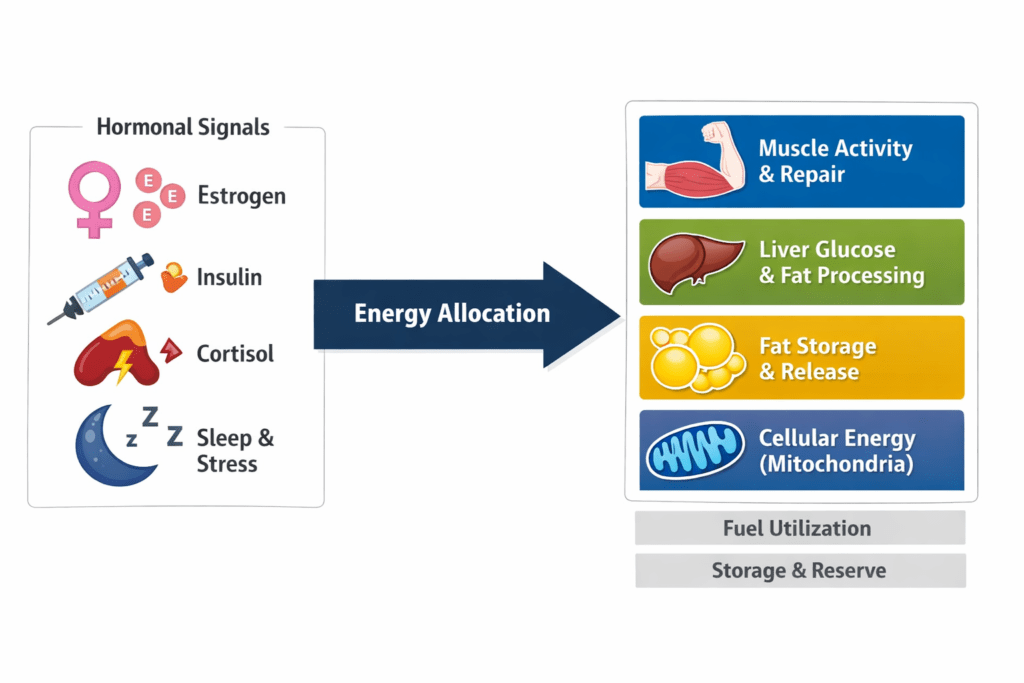
Metabolism is an allocation problem. Your body constantly decides where energy goes, toward movement, repair, immune activity, thermoregulation, reproduction, or storage for later.
Mitochondria sit close to the center of that decision-making, not because they control this process, but because they convert fuel into usable cellular energy and help coordinate signals about energy status. When mitochondrial capacity and quality control are supported, tissues generally handle metabolic stress, meals, missed sleep, demanding training blocks, more smoothly. When capacity is strained, the same stressors can feel metabolically “louder.”
Estrogen as an Energy-Allocation Signal
Estrogen signaling is deeply connected to metabolic regulation in multiple tissues. In skeletal muscle, estrogen receptor signaling has been linked to mitochondrial function, substrate use, and insulin action, one reason researchers pay close attention to the menopausal transition as a metabolic inflection point. (PMC)
This doesn’t mean menopause “causes” poor metabolic health. It means the system’s baseline settings shift, so lifestyle inputs like strength training, sleep, and dietary patterns may matter even more for preserving metabolic flexibility.
Why Visceral Fat Behaves Differently
Not all fat tissue acts the same. Subcutaneous fat (under the skin) can be a relatively safer storage depot in many contexts, while visceral fat (around internal organs) is more strongly associated with insulin resistance and cardiometabolic risk factors.
Across the menopausal transition, many women experience changes in body composition and fat distribution, with research frequently observing increases in waist circumference and central adiposity after menopause. (ScienceDirect)
Why this matters: where energy is stored can influence how inflammatory signals and free fatty acids reach the liver and other organs, shaping cardiometabolic risk over time.
Key Life Stages That Reshape Metabolic Risk
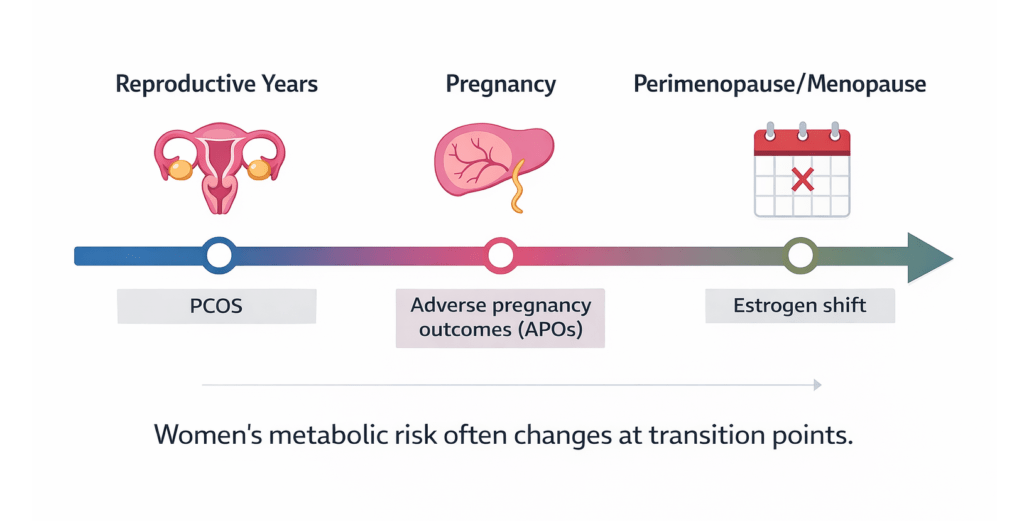
1) Reproductive Years: PCOS as a Metabolic Signal Pattern
Polycystic ovary syndrome (PCOS) is one of the clearest examples of how reproductive hormones and metabolism intertwine. Many (not all) women with PCOS experience insulin resistance, higher rates of metabolic syndrome features, and a higher burden of cardiometabolic risk factors, though the strength of associations can vary by phenotype and body composition. (OUP Academic)
International evidence-based guidelines emphasize comprehensive risk assessment and long-term health considerations in PCOS, because it’s not just a fertility story. (OUP Academic)
Why this matters: PCOS can act like an early “flag” that a person’s metabolic system may benefit from earlier attention to sleep, activity, nutrition quality, and recovery capacity.
2) Pregnancy: A Metabolic Stress Test With Long Shadows
Pregnancy is a normal physiologic state but it’s also a profound metabolic challenge. The body naturally becomes more insulin resistant later in pregnancy to help prioritize nutrient delivery to the fetus. In that context, complications like gestational diabetes or hypertensive disorders of pregnancy can reveal underlying susceptibility and are associated with higher future cardiometabolic risk. (American Heart Association Journals)
This is why many cardiovascular and women’s health groups increasingly treat adverse pregnancy outcomes as important history, not as a cause of future disease on their own, but as valuable information about long-term risk and monitoring needs. (American Heart Association Journals)
Why this matters: pregnancy history can be one of the earliest, most meaningful data points for a woman’s long-term metabolic trajectory.
3) Perimenopause and Menopause: When Fuel Partitioning Often Changes
During the menopausal transition, estrogen levels fluctuate and then decline. Many women notice changes in appetite regulation, sleep, body composition, and recovery. Research commonly observes increases in central adiposity and shifts in adipokines and related signals after menopause, though individual responses vary widely. (ScienceDirect)
Some research has explored how menopausal hormone therapy (MHT) relates to body composition and metabolic measures, but this is nuanced and individualized; major guidelines emphasize weighing benefits and risks based on symptoms, age, timing, and personal risk factors. (OUP Academic)
Why this matters: menopause is often a “metabolic pivot,” where foundations like strength training and sleep can have outsized returns.
How a Metabolic Strategy Can Shift by Life Stage
- Reproductive years: Some women benefit from emphasizing muscle, sleep consistency, and balanced meals to support steady energy and glucose control.
- Pregnancy & postpartum: Recovery capacity often becomes the limiting factor, so routines may need to be simpler and more flexible.
- After pregnancy complications (like gestational diabetes or hypertensive disorders): Many guidelines treat these as useful history for long-term risk conversations with a clinician.
- Perimenopause & menopause: Changes in sleep, body composition, and fat distribution are common, and strength training plus sleep support often become even more important.
- Any stage: Lifestyle foundations come first; a targeted supplement like Mitozz can be considered as support to your overall strategy.
A Simple Metric That’s Often More Informative Than the Scale
If you’re looking for a practical marker often used in research and clinical screening, waist circumference is frequently more aligned with visceral fat risk than weight alone (though it’s still imperfect). Metabolic syndrome definitions commonly include central obesity/waist criteria and related markers like triglycerides, HDL, blood pressure, and fasting glucose. (International Diabetes Federation)

Important note: cutoffs can vary by guideline and ethnicity, and no single metric diagnoses metabolic health by itself. The goal is context not labeling.
Four Levers That Reliably Influence Metabolic Flexibility
1) Muscle: the “glucose sink” and metabolic buffer
Skeletal muscle is one of the largest sites for glucose disposal after meals. Building and maintaining muscle through resistance training supports insulin sensitivity and provides metabolic reserve, especially valuable during perimenopause and beyond, when body composition tends to shift.
Why it matters: more muscle and better mitochondrial capacity can make the same carbohydrate load feel “smaller” to the system.
2) Sleep and circadian timing: an underestimated insulin lever
Sleep isn’t passive downtime. It’s metabolic coordination time. Controlled sleep restriction research in women has shown reduced insulin sensitivity after chronic insufficient sleep, with particularly notable effects reported in postmenopausal women in some studies. (PubMed)
Why it matters: if sleep is chronically short, nutrition and exercise have to work harder to create the same metabolic outcome.
3) Nutrition patterns that support fuel switching
Rather than obsessing over a single macronutrient ratio, think in terms of fuel handling:
- Prioritizing protein adequacy (to support muscle and satiety)
- Fiber-rich carbohydrate sources (to slow glucose spikes and support gut signaling)
- Meal timing that fits sleep and training demands
In postmenopausal women, reviews emphasize lifestyle interventions like diet quality and physical activity as central pillars for healthier adipose tissue function and body composition. (Exploration Publishing)
4) Stress, recovery, and inflammation tone
Chronic psychological stress can elevate behaviors and physiologic signals (sleep disruption, cortisol dynamics, appetite cues) that indirectly shape insulin sensitivity and fat distribution. This frames recovery as a biological input, not a luxury.
Where Targeted Nutritional Support May Fit
Once the foundations are in place, some people explore targeted compounds that have been studied in relation to mitochondrial signaling and metabolic physiology.
Mitozz is a nutraceutical developed by FMG Health Sciences that contains (-)-epicatechin, a compound researchers have investigated for their role in cellular signaling pathways related to mitochondrial function and metabolic regulation.
Conclusion
Women’s metabolic health isn’t a fixed label. It’s a moving balance between hormonal signals, mitochondrial capacity, muscle, sleep, and the transitions that reshape physiology over time. PCOS may show up as an early metabolic clue, pregnancy can reveal hidden vulnerability under demand, and menopause often changes how the body partitions fuel and stores fat.
These shifts don’t define your metabolic destiny but they can change which habits matter most right now, because metabolism doesn’t respond the same way in every life stage.
If you would like to read more about how to improve mitochondrial health, consider exploring our article How to Repair and Maintain Mitochondrial Health Naturally.
Share this blog article
Understanding mitochondrial health is a long-term process and that’s why we created the Mitozz Community. It’s is a free space to explore the science of cellular energy, learn how lifestyle signals support mitochondria, and stay informed through expert discussions, educational content, and live Q&A—at your own pace.
Join the Mitozz Community
Access member and expert discussions, educational content, and live Q&A sessions focused on cellular energy and mitochondrial health.
Medical Disclaimer: The information provided in this article is for educational and informational purposes only and is not intended as medical advice. It is not a substitute for professional medical diagnosis, treatment, or guidance. Always consult with a qualified healthcare professional before making changes to your diet, exercise routine, fasting practices, or supplement use, especially if you have a medical condition, are pregnant or nursing, or are taking medications.
FDA Disclaimer: These statements have not been evaluated by the Food and Drug Administration. They are not not intended to diagnose, treat, cure, or prevent any disease.






