Key Takeaways
- Female metabolism isn’t “random,” it’s responsive to hormones, sleep, stress, training load, and fueling.
- After ovulation, a small temperature shift can subtly change sleep, appetite, and recovery.
- The luteal phase may raise resting calorie burn a little but the bigger story is how you feel.
- The “harder days” are often predictable once you track a few signals.
- A few small adjustments can make your energy feel steadier than you’d expect.
The hidden reason your metabolic “baseline” keeps moving
Most wellness advice assumes women’s metabolism is a steady backdrop. You eat a certain way, train a certain way, and your energy should line up predictably, however, many women notice that real life does not fall in line with this expectation. Some days you feel unstoppable on the same breakfast and the same sleep. Other days, you feel hungrier, puffier, warmer, or oddly flat in workouts with no obvious explanation.
One underappreciated reason for this is that female physiology often runs on a shifting internal context. Across a menstrual cycle, hormones can influence temperature regulation, appetite signaling, fluid balance, and how the body prefers to use fuels. Metabolism is not “random”, it is responsive.
A simple map of cycle phases and hormones
Every cycle is unique but a useful high level map looks like this:
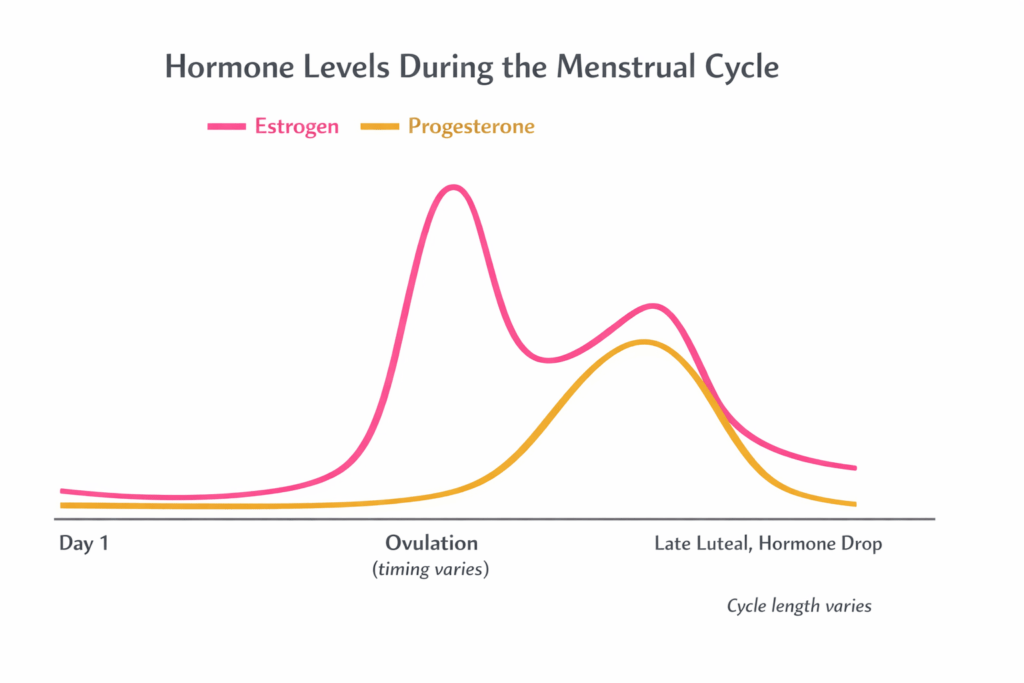
- Follicular phase: Starts on day 1 of bleeding and continues up to ovulation. Estrogen rises.
- Ovulation: A relatively brief event.
- Luteal phase: The post ovulation phase. Progesterone rises and estrogen has a secondary bump. If pregnancy does not occur, both hormones fall in the late luteal phase, which is when many women experience PMS symptoms.
Two important caveats: Not every cycle includes ovulation and cycle length can vary widely. That variability is why the same “day” of the month can feel different across different months.
What changes across the month
Resting metabolic rate and body temperature
If you have ever felt warmer at night after ovulation, you are not imagining it. Progesterone is associated with a rise in core body temperature, and that thermogenic shift is one reason researchers have looked at resting metabolic rate across the cycle.
A 2020 systematic review and meta analysis found a small but statistically significant increase in resting metabolism in the luteal phase compared with the follicular phase. (PMC) The key word is small. This does not mean you “burn hundreds more calories” every day but it can help explain why some women feel a little warmer, a little more restless at night, or slightly more calorie seeking after ovulation.
Why this matters: When your physiology nudges energy expenditure and temperature up, your sleep quality, appetite, and recovery signals may shift too, even if your routine does not.
Appetite and cravings
Many women report higher hunger and more cravings in the late luteal phase. Research broadly supports that energy intake often increases in the luteal phase of ovulatory cycles, though measurement methods and phase confirmation matter. (PMC)
You shouldn’t think of cravings as a “lack of willpower.” Appetite is regulated by a network of brain, gut, and adipose signals that are sensitive to hormones, sleep, stress, and training load. Cycle phase can be one more variable nudging that network.
Why this matters: If you treat luteal hunger as a personal failure, you may overcorrect with restriction, which can backfire on mood, sleep, and training quality. A better strategy is to anticipate the pattern and support it with a smarter structure.
Glucose handling and perceived “carb tolerance”
Some women notice that glucose swings feel different across the month. The literature here is complex and can be population specific. A systematic review focused on type 1 diabetes highlights that menstrual cycle effects on glycemic outcomes and insulin sensitivity can be difficult to generalize because methods vary and individual responses are heterogeneous. (PMC) Additional research has discussed phase dependent differences in insulin related brain signaling and glucose control but the practical takeaway remains individualized monitoring rather than assuming a universal rule. (The Lancet)
Why this matters: If your energy dips or cravings spike, it may not be because you are “bad at carbs.” It may be that sleep, stress, training load, and cycle phase are interacting.
Fluid balance, scale weight, and GI-related changes
Late luteal changes often include water retention and shifts in gastrointestinal comfort. (PMC) This can change scale weight, how rings fit, and how “puffy” you feel, without reflecting fat gain. (Springer Link) Late luteal hormone withdrawal can also alter perceived soreness and mood in some people, which can change how training feels.
Why this matters: If you react to a few days of water-driven scale changes by cutting calories or increasing training aggressively, you can disrupt recovery and make your overall plan harder to sustain. Short-term fluctuations don’t require long-term corrections.
Exercise performance and recovery
Performance is multifactorial and not every woman notices clear phase effects. Still, researchers have explored how substrate use and training responses may vary across phases, partly due to hormone effects on fuel utilization and thermoregulation. (MDPI)
A more useful framing is that your baseline fitness hasn’t changed, but your recovery status and fuel availability can fluctuate. Sleep, stress, glycogen, hydration, and hormonal context all shape how training feels on a given day.
Why this matters: Adjusting intensity and volume to match your recovery status and fuel availability helps maintain consistency and reduce unnecessary fatigue. Forcing the same plan every week can do the opposite.
Why mitochondria matter
Mitochondria are where cells convert nutrients into usable energy and they also participate in signaling that influences adaptation, stress responses, and metabolic flexibility. (PubMed) Estrogen related signaling has been discussed in relation to mitochondrial function and muscle metabolism in review level work, particularly across life stages such as menopause. (Physiological Journals)
It is tempting to reduce everything to “hormones change mitochondria, therefore you feel tired,” however, real physiology is more layered. Hormones influence temperature, sleep, appetite, fluid balance, and the nervous system, and those variables shape how mitochondria are supplied with oxygen, substrates, and recovery signals.
A more practical way to think about it is that mitochondria reflect the conditions you give them. They integrate signals from across the body rather than operating in isolation.
This helps explain why the same workout can feel different across the month, even when your underlying fitness hasn’t changed.
Practical ways to work with cycle based variability

1. Track, don’t guess
If you want clarity, track a few simple signals for two to three cycles including, cycle day, sleep quality, hunger, training performance, and mood. If you can confirm ovulation (for example, with basal temperature patterns or other methods), your phase map becomes much more accurate.
2. Treat the luteal phase like a recovery phase
If you tend to run warmer, sleep worse, or feel hungrier after ovulation, build in small supports:
- Earlier wind down
- Slightly more calories from protein and fiber rich carbs
- More hydration.
The goal is not perfection, it is reducing friction.
3. Use “readiness based” training
Keep your workout plan, just adjust the dial. Think of readiness as how prepared your body feels on a given day, based on things like sleep, energy, soreness, stress, and how well you’re fueled and hydrated.
On higher-readiness days, lift heavier or push intensity. On lower-readiness days, keep the habit but reduce volume, prioritize technique, or do zone 2 cardio and mobility. This preserves consistency without fighting your biology.
4. Treat scale changes as data, not verdicts
If your weight rises 1 to 3 pounds in late luteal days, consider that to be water retention and gastrointestinal shifts first, not fat gain. Hormonal changes during this phase can influence fluid balance and digestion, which can temporarily affect scale weight.
Look at trends across the month, not just single days. A single reading is a snapshot, not a conclusion.
5. Remember that life stage matters
Perimenopause and menopause change your body’s hormonal landscape. If your cycle is irregular or you are in a transitional stage, variability can increase. The same principles apply, track signals, support sleep, strength train, and prioritize recovery, but your expectations should be flexible.
How to use your cycle signals
Over time, the signals you track become patterns you can act on. Use them to make small adjustments in training, recovery, and nutrition rather than guessing day to day.
| Signal | Adjustment |
|---|---|
| Low energy, poor sleep | Reduce training volume, keep intensity moderate, prioritize sleep and hydration. Often reflects lower recovery capacity. |
| Higher hunger | Add slightly more calories if needed, especially from protein and fiber-rich carbohydrates. This may reflect a phase where appetite rises and recovery support matters more. |
| Increased soreness | Keep the training habit but shift toward technique work, mobility, or zone 2 cardio. This often means recovery is lagging, even if baseline fitness has not changed. |
| Feeling puffy or heavier | Treat it as water retention and gastrointestinal shifts first, not fat gain. Look at monthly trends, not single weigh-ins, and avoid aggressive diet changes. Short-term scale movement does not always require correction. |
| High energy, strong performance | Push intensity, lift heavier, or take advantage of the day for harder work. This often reflects better recovery status, stronger fuel availability, and higher readiness. |
Where Mitozz fits in
The lifestyle foundations of sleep, training, nutrition, and stress management, remain the biggest levers for metabolic resilience. For readers who want to explore targeted nutritional support, Mitozz is a nutraceutical developed by FMG Health Sciences that contains 98% pure (-)-epicatechin, a compound studied in the broader science literature for its role in cellular signaling pathways linked to mitochondrial related function and metabolic adaptation.
This is relevant because mitochondria help convert nutrients into usable energy and coordinate recovery signals, systems that can feel more “sensitive” during phases like the post-ovulation luteal window when body temperature and perceived energy needs may shift. Mitozz is best viewed as complementary support, not a substitute for the fundamentals, and tends to be the most effective when stacked consistently with sleep, training, and nutrition habits over time.
Conclusion
Female metabolism is not a fixed number, it’s a responsive system shaped by hormones, sleep, stress, training load, and energy availability. While research suggests only small average increases in resting metabolic rate and often higher appetite in the luteal phase, the most useful insight is practical.
Learn your pattern.
Track a few key signals, anticipate your predictable friction points, and use flexible habits that help keep energy and recovery steadier across the month. Your baseline capacity doesn’t disappear, the conditions around it shift.
If you want to go deeper, especially on how daily habits support more stable energy at the cellular level, read our article How to Repair and Maintain Mitochondrial Health Naturally, where we break down practical strategies to support mitochondrial function through sleep, nutrition, movement, and recovery.
FAQs
Does metabolism increase in the luteal phase?
Yes, often slightly (on average).
- RMR tends to be a bit higher after ovulation
- Likely linked to progesterone and higher core temperature
- The change is small and varies a lot person to person
Why do I feel hungrier before my period?
Because late luteal physiology can nudge appetite up.
- Hormone drop (estrogen, progesterone) can affect mood and cravings
- Warmer nights can disrupt sleep, which can increase hunger
- Many women simply have higher drive to eat in this window
Does insulin sensitivity change across the menstrual cycle?
Sometimes, but not consistently for everyone.
- Best approach: track your pattern (cycle day + sleep + stress + meals)
- Some people see more glucose swings in the luteal phase
- Research findings are mixed and highly individual
Why does my weight fluctuate before my period?
Mostly water and gut shifts, not fat gain.
- Fluid retention can increase late luteal
- GI changes can affect scale weight
- Compare trends month-to-month in the same cycle window
Do hormonal contraceptives change these patterns?
Yes, they can change or blunt typical cycle patterns.
- Many methods suppress ovulation
- Symptoms and “phases” may be different or less predictable
- Track your lived pattern rather than assuming standard phases
Share this blog article
Understanding mitochondrial health is a long-term process and that’s why we created the Mitozz Community. It’s is a free space to explore the science of cellular energy, learn how lifestyle signals support mitochondria, and stay informed through expert discussions, educational content, and live Q&A—at your own pace.
Join the Mitozz Community
Access member and expert discussions, educational content, and live Q&A sessions focused on cellular energy and mitochondrial health.
Medical Disclaimer: The information provided in this article is for educational and informational purposes only and is not intended as medical advice. It is not a substitute for professional medical diagnosis, treatment, or guidance. Always consult with a qualified healthcare professional before making changes to your diet, exercise routine, fasting practices, or supplement use, especially if you have a medical condition, are pregnant or nursing, or are taking medications.
FDA Disclaimer: These statements have not been evaluated by the Food and Drug Administration. They are not not intended to diagnose, treat, cure, or prevent any disease.






