Puntos clave
- Feeling tired “for no reason” is often a systems issue, not a willpower issue.
- Daily energy depends on cellular fuel-making and fuel-allocation, especially under stress.
- Sleep is when your body restores capacity and relieves sleep pressure.
- Routine labs can rule out big problems but often miss day-to-day recovery strain and energy regulation.
- Mitozz is a great targeted supplement support if you always feel tired.
You know the feeling, you wake up and your day hasn’t even started yet but you already feel like you’re behind. Coffee helps but it doesn’t really get you to where you want to be. On paper your habits look fine, but somehow, your energy isn’t what it should be.
If that sounds familiar, you are not alone. Fatigue is one of the most common reasons people seek help from primary care and it can show up even when basic checklists look “fine.” (AAFP)
Why am I always tired even when everything seems normal?
You can feel tired even when your sleep, diet, and routine look normal because energy is produced at the cellular level. When your body’s energy systems are under strain, from stress, poor recovery, or metabolic inefficiency, energy can feel low even without an obvious cause.
This doesn’t mean something is wrong with you. It can mean your system is running closer to its limits than you realize.
Signs Your Energy System mayo Be Underperforming
- You wake up tired even after a full night of sleep
- You rely on caffeine just to feel normal
- You crash in the afternoon
- You feel mentally slow, foggy or unfocused
- Your workouts feel harder than they should
These signs can point to how well your body is matching energy supply to daily demand.
The missing layer, energy is made inside cells
When people think about energy, they usually think about inputs like, sleep, food, motivation. But your lived experience of energy depends on something more basic, how well your cells can turn those inputs into steady, usable fuel, minute to minute.
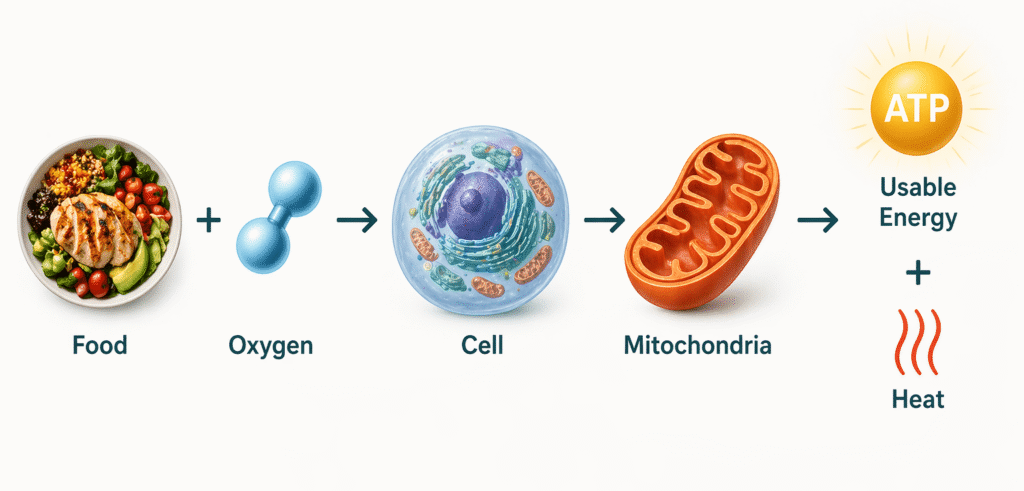
That is where mitochondria come in. Mitochondria are organelles inside most of your cells that help convert nutrients and oxygen into ATP, the main form of usable cellular energy for all bodily functions. They also help coordinate signaling around stress, inflammation, and adaptation. (ScienceDirect)
Mitochondria are your “power plants” and more
The power-plant analogy helps, but it misses a very important point. Mitochondria don’t just output energy, they sense demand and adjust capacity. Their performance shifts with sleep, training, stress load, and illness, which is why energy can feel unpredictable even when your routine looks “normal.” (PMC)
One of the clearest examples that mitochondria can influence how we feel is fatigue. In mitochondrial dysfunction, fatigue is a common and often prominent symptom, which makes intuitive sense when the machinery that helps produce ATP is impaired. In broader, everyday fatigue, the same biology is usually subtler, more about capacity and efficiency under cumulative strain than a single broken part. (PMC)
And here’s a striking research detail that ties this back to sleep. A 2025 Nature paper found that, in fruit flies, the buildup of sleep pressure is closely linked to mitochondrial bioenergetics in identified sleep-control neurons in the brain. It’s not direct evidence in humans, but it supports the idea that sleep drive and daytime energy can be influenced by cellular energy state, not only by how many hours of sleep you got. (Nature)
Efficiency matters, not just inputs
Two people can sleep the same hours and eat similar meals but feel very different. Part of that gap can come from energy efficiency, how well the body regulates glucose, how well tissues recover, and how much physiological “background load” is eating into capacity. (ScienceDirect)
Surface causes vs deeper causes of fatigue
| Surface Level | Deeper Layer |
|---|---|
| Not enough sleep | Poor cellular recovery |
| Bad diet | Inefficient energy use |
| Stress | Altered energy signaling |
| Lack of exercise | Low mitochondrial capacity |
This doesn’t mean mitochondria explain everything. It’s shows that different everyday triggers, poor sleep, stress, diet swings, low activity, often feed into the same underlying issues of reduced energy capacity and recovery efficiency.
So why doesn’t this show up on tests?
Routine snapshot labs like a CBC, thyroid screening (TSH), iron markers, metabolic panel, and glucose markers, are useful for ruling out common medical causes, but they aren’t designed to measure real-time cellular energy efficiency.
That is why everything can look “normal” but you still feel off. Primary care guidelines note that fatigue is common, causes are often multifactorial, and labs do not always reveal a single explanation. (AAFP)
If your fatigue is persistent, worsening, or paired with concerning symptoms, it is worth discussing with a qualified clinician. “Normal” labs do not always rule out sleep disorders, mood factors, medication effects, iron issues, thyroid problems, or other common contributors. (AAFP)
4 common “normal life” pressures that drain energy capacity
1) Sleep debt and circadian mismatch
You can get enough hours of sleep but still get low quality recovery. Fragmented sleep, late nights, irregular schedules, and circadian misalignment can shift hormones and metabolism in ways that change daytime energy. (ScienceDirect)
There is also growing evidence that sleep loss affects peripheral tissues like skeletal muscle, including mitochondrial-related pathways and metabolic function. (PMC)
What this means in real life is simple. If your mornings feel heavy and your afternoons fall apart, it is often less about willpower and more about recovery biology.
Sleep is one of the strongest drivers of how your body recovers at the cellular level. If this process is disrupted, energy production can suffer.
Related Blog Article: What Happens to Your Mitochondria When You Don’t Sleep Enough?
2) Stress load and constant “on” signaling
Stress is not just a feeling. It is a coordinated biological response that changes how your body allocates energy, including through neuroendocrine and immune signaling.
Reviews have described meaningful connections between psychological stress and mitochondrial structure and function, though the direction and magnitude can vary by context and duration. (PMC)
If you live in a constant low-grade sprint, your body can start prioritizing “getting through today” signaling over deep recovery. The result can feel like wired-but-tired, or like you are running on backup power.
Related Blog Article: Cellular Health and Stress Management: How to Protect Your Energy, Recovery, and Resilience
3) Metabolic strain and glucose swings
Energy is not only about how much you eat, it is about how steadily you can use the nutrients in the food you eat. Big gaps between meals, highly refined meals, and low movement can all create bigger rises and drops in blood glucose, which can change perceived energy and focus.
Sleep disruption can also worsen metabolic regulation, which can feed back into energy stability across the day. (ScienceDirect)
If you suffer from afternoon crashes, consider that it is often a combined circadian dip plus metabolic demand plus stress. Fixing one lever can help, but stacking small levers can work better.
4) Deconditioning and low mitochondrial capacity
Mitochondria adapt to demand. Regular aerobic and resistance training can increase mitochondrial capacity and efficiency in muscle, which can translate to better resilience, not just better fitness. When activity drops, capacity can drift downward surprisingly fast.
That’s one reason you can be “doing everything right” and still feel tired. If your baseline capacity has quietly slipped during a stretch of lower movement, the same day can feel heavier, even when your routine looks good on paper. (PubMed)
What actually improves energy stability
If fatigue is not explained by a clear medical cause, the most reliable improvements can usually come from the foundations that increase capacity and reduce background load.
- Sleep consistency. Same wake time most days, wind-down light, and fewer late-night swings. Over weeks, consistency often matters more than perfection.
- Daily movement, even on low days. Short walks after meals, brief strength sessions, and a “minimum dose” mindset support metabolic stability and conditioning.
- Protein and fiber anchored meals. This tends to smooth energy variability for many people, even without strict dieting. This is general nutrition guidance, but since we are all different, individual results will vary.
- Stress downshifts you can repeat. Short, repeatable practices, breathing, daylight, social decompression, can reduce perceived load and improve sleep quality, which feeds recovery.
If you are thinking, “I already do some of this,” that is fine. Energy is often a stack of 5 percent improvements that add up. For a deeper dive into how to improve our cellular energy, read our article, How to Repair and Maintain Mitochondrial Health Naturally.
Where Mitozz fits in
Lifestyle foundations do most of the heavy lifting for energy capacity. That said, researchers are actively investigating compounds that may influence mitochondrial signaling and adaptation.
Mitozz is a nutraceutical developed by FMG Health Sciences that contains 98% pure (−)-epicatechin, a compound studied in relation to vascular and metabolic biology, and mitochondrial-related pathways. If you are building a long-term “energy system,” targeted nutritional support can serve as one of levers in your energy toolkit.
The Bottom Line
If you’re tired all the time, it can feel confusing, especially when your life looks “fine” from the outside.
But energy is not just about sleep hours and calories. It’s about whether your system can convert those inputs into steady, usable fuel, day after day, under real-world stress.
Understanding that energy-production layer can help explain how everyday habits can quietly shape how much energy you actually feel.
Comparte este artículo del blog
FAQs
Why am I always tired even when I sleep 8 hours?
Because sleep duration is not the same as sleep quality or circadian alignment. Fragmentation, late timing, and stress physiology can reduce how restorative sleep feels.
Can stress make you feel tired all day?
Yes. Stress biology changes hormones and signaling that affect recovery, metabolism, and perceived energy. Reviews link psychological stress with measurable mitochondrial-related changes in many studies, though effects vary by context.
Why do I crash in the afternoon?
The afternoon dip is often a mix of circadian rhythm, meal timing, glucose regulation, and accumulated stress load. Sleep disruption can amplify these effects.
Why can my tests look normal but I still feel exhausted?
Common labs often capture broad markers, not moment-to-moment energy regulation, sleep disorders, mood factors, or multifactor load. Clinical guidance notes that fatigue is frequently multifactorial and lab work is not always diagnostic.
Are mitochondria linked to fatigue?
In mitochondrial diseases, fatigue is a core symptom. In broader populations, research supports associations between bioenergetics and fatigue, but this does not mean mitochondria are always the sole cause.
Referencias
- Filler, K., Lyon, D., Bennett, J., et al. (2014). Association of mitochondrial dysfunction and fatigue: A review of the literature. BBA Clinical. (PMC)
- Latimer, K. M., & colleagues. (2023). Fatigue in Adults: Evaluation and Management. American Family Physician (PDF). (AAFP)
- Sarnataro, et al. (2025) Mitochondrial origins of the pressure to sleep. (Nature)
- Picard, M., et al. (2018). Psychological stress and mitochondria: A systematic review. Psychosomatic Medicine. (PMC)
- Picard, M., et al. (2018). An energetic view of stress: Focus on mitochondria. Neuroscience & Biobehavioral Reviews. (ScienceDirect)
- Morrison, M. A., et al. (2022). Sleep, circadian biology and skeletal muscle interactions. Sleep Medicine Reviews. (ScienceDirect)
- Lin, W., et al. (2022). Sleep restriction effects in peripheral tissues including skeletal muscle. (Review/Article, PMC). (PMC)
- Saner, N. J., et al. (2021). Sleep-loss-induced changes in glucose tolerance and mitochondrial function. (PDF). (VU Research)
- Sarnataro, R., et al. (2025). Neurobiology of mitochondrial dynamics in sleep. The Journal of Physiology. (Physiological Society Online)
- Maisel, P., et al. (2021). Fatigue as the chief complaint: Epidemiology, causes, diagnosis, and treatment. Deutsches Ärzteblatt International (PMC). (PMC)
Comprender la salud mitocondrial es un proceso a largo plazo y por eso hemos creado la Mitozz . Se trata de un espacio gratuito para explorar la ciencia de la energía celular, aprender cómo los hábitos de vida favorecen a las mitocondrias y mantenerse informado a través de debates con expertos, contenidos educativos y sesiones de preguntas y respuestas en directo, a tu propio ritmo.
Únete a la Mitozz
Accede a debates entre miembros y expertos, contenidos formativos y sesiones de preguntas y respuestas en directo centrados en la energía celular y la salud mitocondrial.
Aviso médico: La información proporcionada en este artículo tiene fines exclusivamente educativos e informativos y no pretende constituir un consejo médico. No sustituye el diagnóstico, el tratamiento ni la orientación médicos profesionales. Consulte siempre a un profesional sanitario cualificado antes de realizar cambios en su dieta, rutina de ejercicio, prácticas de ayuno o uso de suplementos, especialmente si padece alguna afección médica, está embarazada o en periodo de lactancia, o está tomando medicamentos.
Descargo de responsabilidad de la FDA: Estas declaraciones no han sido evaluadas por la Administración de Alimentos y Medicamentos (FDA). No están destinadas a diagnosticar, tratar, curar ni prevenir ninguna enfermedad.